First study on drug-resistant malaria in Bangladesh
The International Centre for Diarrhoeal Disease Research, Bangladesh, is set to launch the first surveillance study aimed at identifying drug-resistant malaria strains in the Rohingya refugee camps in Cox’s Bazar, a move experts say is crucial to protecting Bangladesh’s progress in malaria control.
The study will be conducted in collaboration with the National Malaria Elimination Programme under the Directorate General of Health Services and development organisation BRAC. Researchers will analyse samples from malaria patients in the camps to detect parasites that may have developed resistance to commonly used treatments.
According to a press release issued on March 11, the initiative comes amid growing concern over the spread of drug-resistant malaria parasites in neighbouring Myanmar. Health experts warn that if such strains enter or spread in Bangladesh, they could undermine the country’s goal of eliminating malaria by 2030.
Malaria is a life-threatening disease transmitted through the bite of infected mosquitoes. The most dangerous form of the disease is caused by the parasite Plasmodium falciparum, which is responsible for the majority of severe cases and deaths worldwide. Although malaria can currently be treated with effective medicines, the emergence of drug-resistant parasites can significantly reduce the effectiveness of treatment and pose major challenges to disease control.
The planned surveillance study will focus on Rohingya camps in Cox’s Bazar, which lie close to the Bangladesh-Myanmar border. Experts say the location makes the camps particularly vulnerable to the introduction and spread of resistant malaria strains through cross-border movement.
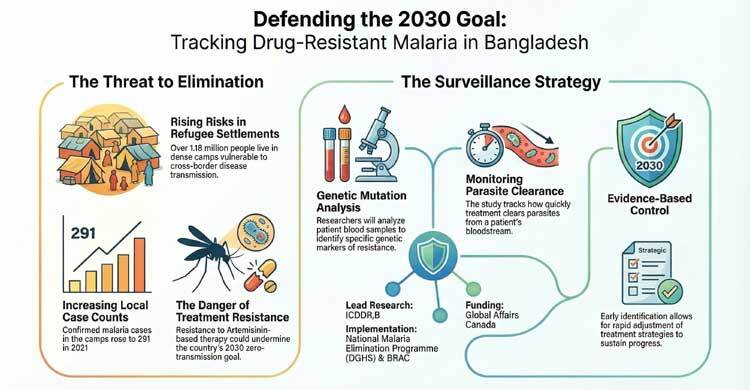
More than 1.18 million Rohingya refugees currently live in 33 camps in the district, making it one of the largest refugee settlements in the world. Dense population, frequent travel and limited health surveillance in some areas increase the risk of disease transmission.
Recent surveillance data collected by BRAC indicate that malaria cases in the camps have risen in recent years. In 2021, a total of 291 confirmed malaria cases were reported in the camps. Most infections were caused by Plasmodium falciparum, with many cases linked to travel to malaria-endemic areas such as Bandarban or cross-border movement from Myanmar.
To discuss the situation and the upcoming study, a coordination meeting was held on March 10 at the office of the Refugee Relief and Repatriation Commissioner in Cox’s Bazar. Representatives from government agencies, research institutions and humanitarian organisations working in the camps attended the meeting.
Refugee Relief and Repatriation Commissioner Mohammad Mizanur Rahman said Bangladesh has made significant progress in controlling malaria over the past decade, but warned that continued vigilance is essential.
“Strengthening surveillance in high-risk areas like Cox’s Bazar will protect both refugees and the local population and ensure effective malaria treatment,” he said.
During the meeting, Dr Md Sirajul Islam, surveillance medical officer of the National Malaria Elimination Programme, highlighted the current malaria situation in the camps and stressed the need to enhance monitoring systems.
Later, Anamul Hasan presented the proposed research plan. He said malaria patients will be enrolled from selected refugee camps and nearby health facilities. Blood samples will be collected and analysed to identify genetic mutations in the parasite that may indicate resistance to treatment.
Researchers will particularly examine resistance to Artemisinin-based combination therapy, the most widely used treatment for malaria worldwide. The study will also monitor how quickly parasites are cleared from patients’ blood after treatment, which is an important indicator of drug effectiveness.
The research project will be funded by Global Affairs Canada, with patient enrolment expected to begin in April.
Dr Mohammad Shafiul Alam, a scientist at icddr,b, warned that drug-resistant malaria could spread unnoticed if not detected early.
“Early identification of resistance and evidence-based strategies for treatment and control are essential to sustaining Bangladesh’s progress in malaria elimination,” he said.
Health experts are also urging residents in malaria-prone areas to seek medical attention immediately if they experience symptoms such as fever, chills, headache or extreme fatigue. Timely testing and completing the full course of prescribed medication remain key to preventing complications and reducing transmission.
Under Bangladesh’s National Malaria Elimination Strategy 2024–2030, the government aims to reduce local malaria transmission to zero by 2030. Experts say strengthening disease surveillance and quickly detecting any emergence of drug resistance will be critical to achieving that goal.

